Journal
This week I have been working in the main department of the Queen Margaret Hospital. This particular department deals with patients being referred from the Accident and Emergency department, ward patients and requests from General practitioners. It was an incredibly busy week and, as always, there were many times that I had to adapt my technique in order to overcome potential difficulties in obtaining an image.
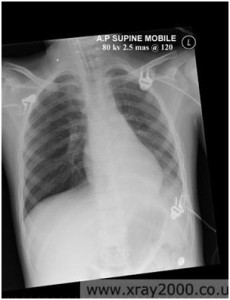
One case in particular that presented a huge challenge with regards to achieving a viable image was a 13 year old girl who had been transferred to the hospital from the “sick kids†hospital in Aberdeen. She had been diagnosed with a comminuted fracture of the left femur and the orthopaedic consultant required an up to date x-ray of her injury.
When she arrived in the x-ray department she was in traction lying on an orthopaedic cot. It was the first time I had seen a cot with all the traction and it was referred to a cot because it looked similar to a baby’s cot except that it had additional poles running along the top. There was also a boom and hoist fitted that allowed the patient to lift herself up.
There are several different types of traction used when treating thighbone fractures. These range from placing the leg in a cast to using sticky tape (skin traction) or metal pins (skeletal traction) in order to attach a series of strings which are in turn attached to weights. X-rays are then used in order to monitor the position of the bone so that the traction can be suitably adjusted.
Working with the radiographer on this particular case we firstly assessed how we were going to position the cassette for the examination. We managed to position the cassette under the patient and raise it at one end to run parallel
to her leg. This allowed the tube above her bed to be angled to the cassette to produce an AP radiograph. This projection was quite difficult for me to achieve for a number of reasons. Firstly, as the bed was quite tall I found myself
climbing onto the x-ray table in order to position the tube correctly. Also thet tube had a longer distance from the cassette than normal due to the bars running horizontally across the top of the bed which restricted the tube from gaining the correct focus to film distance. We overcame this last problem by increasing the mAs in order to achieve a good image.
The lateral projection presented another set of problems mainly due to the position of the metal rods running down the medial and lateral sides of the leg. The radiographer suggested that we try and obtain an oblique image, as the
previous lateral image did not show the displacement of the fracture very clearly. We agreed on this strategy and I slipped a foam pad under the patient, raising her off the bed, and positioned the cassette. The patients fracture was
in the lower two-thirds of her femur so the cassette was placed vertically on the medial aspect of the leg for a horizontal beam lateral (HBL). The radiographer positioned the tube for a HBL and then added an angle to the tube in order to try and displace the traction rods form obscuring the bone and the fracture. The resulting image was not as good as he would have liked due to the traction still obscuring part of the fracture, however, it did show most of the fracture and he felt that there was no need to repeat the examination.
I found this week to be a great learning experience. Trying different positions due to various obstacles such as restricted patient movement and the orthopaedic traction bed really helps to develop my experience and expertise as a radiographer.